|
To better understand a vaccine’s side effects, consider what happens when we get vaccinated. Each one of us makes a different kind of immune response.” Age, sex, genetics, preexisting conditions, environment and even our diet influences how our immune systems might react, she says. “But at the same time, just because a person didn’t feel anything doesn’t mean the immune response wasn’t vigorous. “If you really feel it, you’re mounting a really vigorous immune response,” says Sujan Shresta, a viral immunologist at the La Jolla Institute for Immunology. But ultimately, the experience probably reflects the quirks of each person’s immune system more than it does the vaccine’s effectiveness. So why do some people get side effects and others do not? “It’s a great question, and we don’t know the answer,” Wherry says. “The big take-home message is that not having side effects, or not as severe side effects, is no reason to worry,” says John Wherry, an immunologist at the University of Pennsylvania. Yet only about half of trial subjects experienced the sort of systemic reactions that Duehmig did. The latter indicated that the vaccine was generally 90 to 100 percent effective against COVID-19 in people regardless of their sex, age, race, ethnicity or preexisting conditions. So was Griesar’s vaccine any less effective at protecting him from severe COVID-19?Ībsolutely not, according to experts and data from clinical trials of the Pfizer vaccine. “I do like to think that it means it’s working, that it’s kicking my system into gear,” Duehmig says. “I really didn’t want to do anything but sleep that day, which is about all I did.” with the chills and some body aches and just not feeling well by the morning,” Duehmig says. But for Duehmig, the effects were more pronounced. After the jab, Griesar felt nothing more than a sore arm. These reports could help guide clinical assessment and management of autoimmune manifestations after COVID-19 vaccination.ĬOVID-19 SARS-CoV-2 adverse events autoimmune diseases vaccines.Last month Robert Duehmig and Bill Griesar-a married couple in their 50s who live in Astoria, Ore., and Portland, Ore.-were each relieved to get their second shot of the Pfizer-BioNTech vaccine for COVID-19. In fact, we do not aim to disavow the overwhelming benefits of mass COVID-19 vaccination in preventing COVID-19 morbidity and mortality. Although information pertaining to the risk of autoimmune disease as a consequence of vaccination is controversial, we merely propose our current understanding of autoimmune manifestations associated with COVID-19 vaccine. Here, we summarize the emerging evidence about autoimmune manifestations occurring in response to certain COVID-19 vaccines. However, whether the association between COVID-19 vaccine and autoimmune manifestations is coincidental or causal remains to be elucidated. 
Molecular mimicry, the production of particular autoantibodies and the role of certain vaccine adjuvants seem to be substantial contributors to autoimmune phenomena. 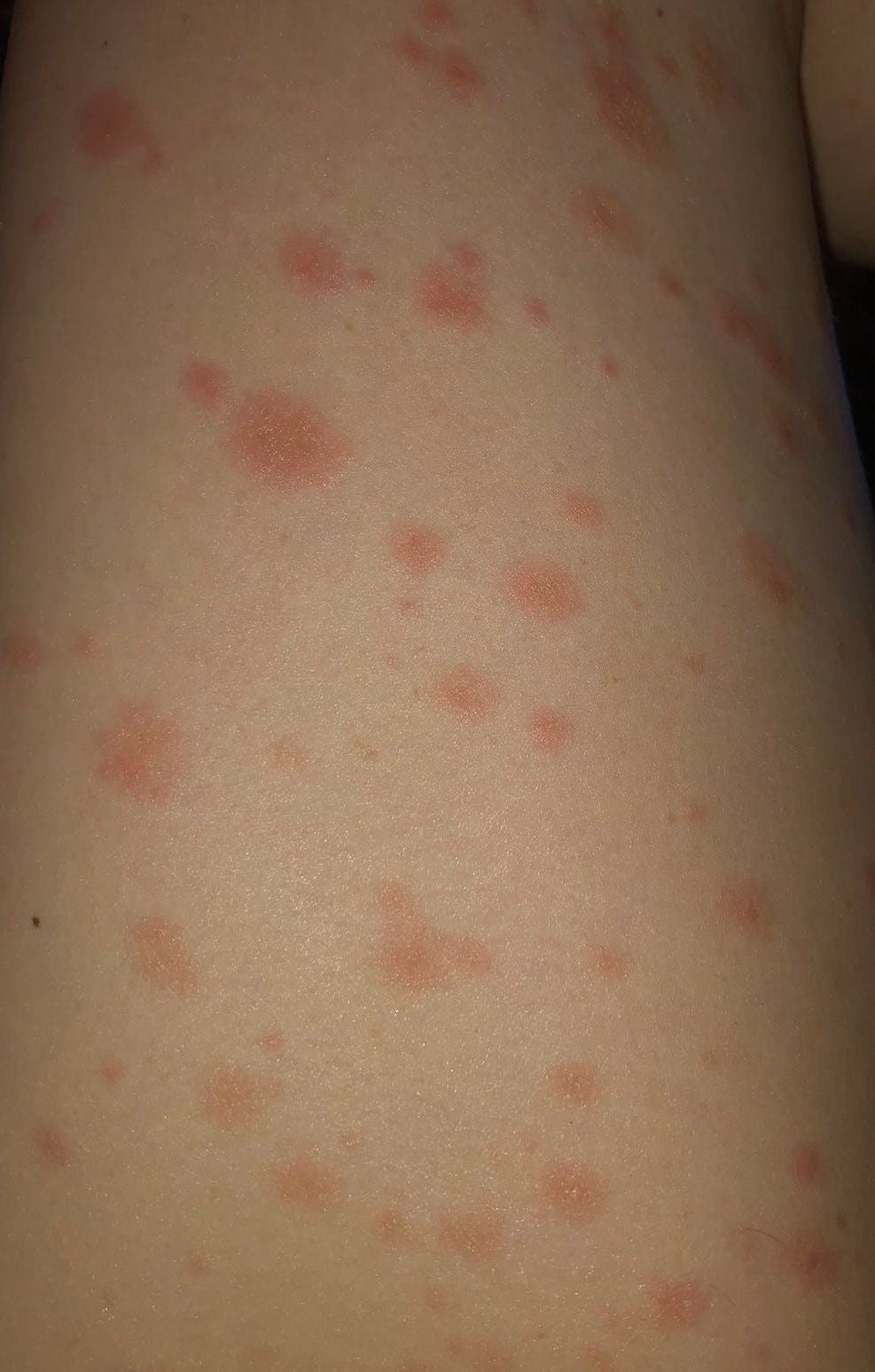 
immune thrombotic thrombocytopenia, autoimmune liver diseases, Guillain-Barré syndrome, IgA nephropathy, rheumatoid arthritis and systemic lupus erythematosus). Recently, new-onset autoimmune phenomena after COVID-19 vaccination have been reported increasingly (e.g. Vaccination programmes are being rolled out globally, but most of these vaccines have been approved without extensive studies on their side-effects and efficacy. Vaccination is one of the most effective interventions to substantially reduce severe disease and death due to SARS-CoV-2 infection. Coronavirus disease 2019 (COVID-19) pandemic caused by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) has led to an unprecedented setback for global economy and health.
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
